Looking Bravely: Breastfeeding Education in Nepal

We recently spoke with Nisha Sharma, a specialist in child feeding in Nepal. Since joining Helen Keller Intl in 2010, Nisha has conducted research about breastfeeding practices, the marketing of baby formula, and other issues with the dual goals of influencing public policy and further enhancing our evidence-based support for mothers and infants.
Her role as Research Manager for Assessment & Research on Child Feeding (ARCH) is influenced by both professional and personal experience.
Nisha and the rest of her team focus on improving nutrition during the first two years of life — a crucial window of opportunity to shape a child’s future. Good nutrition during this time helps babies grow, feeds intelligence, and provides the foundation for a healthy and productive life. Nisha’s work promotes these efforts, helping future generations receive the nutritional support they need from the moment they’re born.
Why is it so important to work on both policy and programming?
Firm regulations are needed from the government, because any loopholes in policy can mean someone will take advantage. Companies that make baby formula often make use of gaps in regulations to market a product misleadingly, for example, incorrectly labeling the amount of nutrients contained. But just having good policy is not enough. Trained health workers must put policies into action.
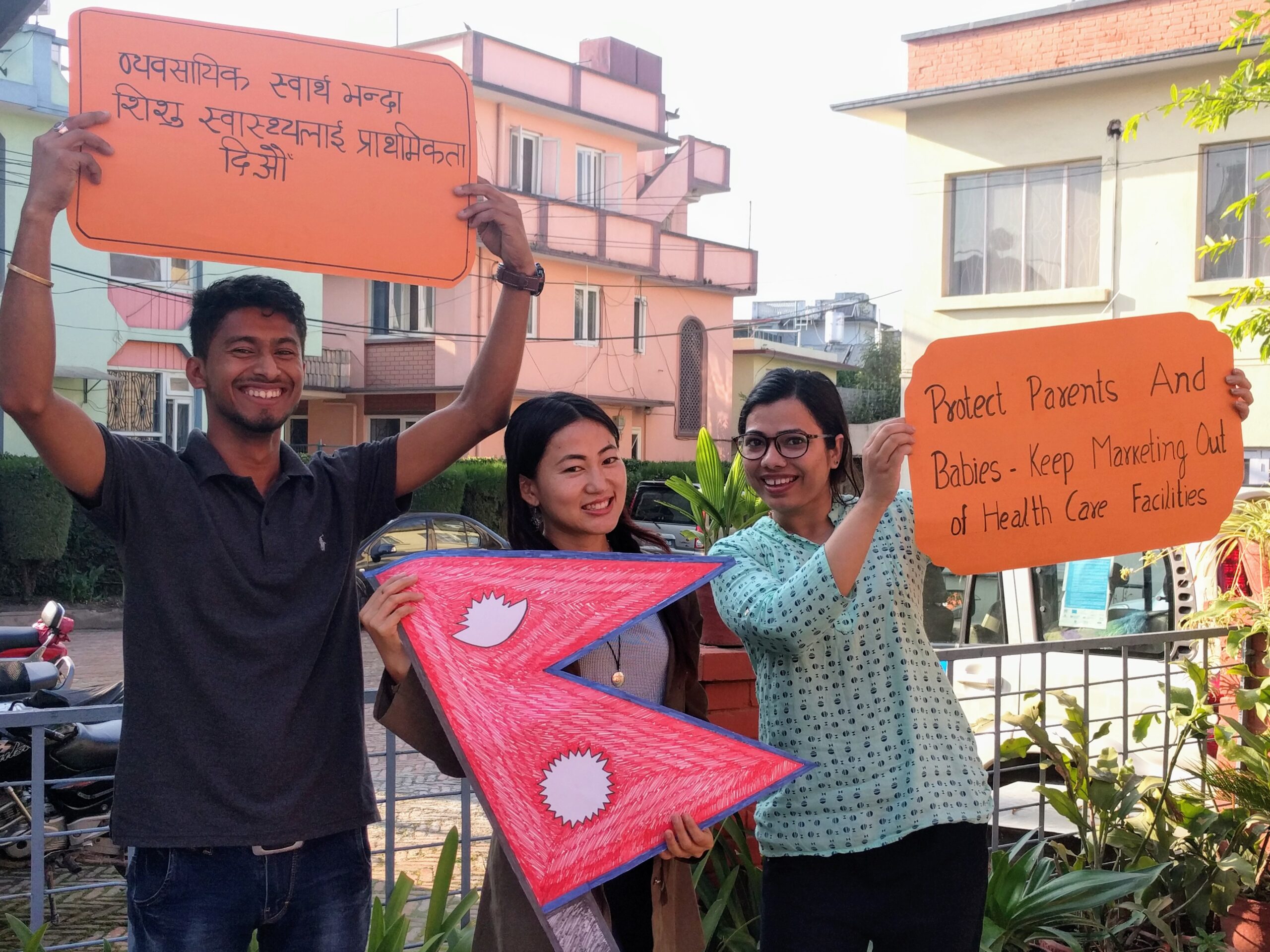
How do you work to close gaps in knowledge about breastfeeding?
Acknowledging that breastmilk is the most nutritious food for babies under six months, Nepal’s government does promote breastfeeding. And almost all mothers here breastfeed. The problem lies in not understanding exclusive breastfeeding.
When we began training in hospitals, nurses would say, “Everyone knows about breastfeeding. Why do we need training?” But in interviews, we heard many misconceptions. For example, when we asked how much breastmilk a newborn needs per feeding, many said 30 mL [1 oz], which is almost six times the right amount!
Many private hospitals have protocols for separating a mother from her infant after delivery. But it is very important that a baby start breastfeeding within one hour of birth. If you miss that window, it becomes more difficult for the baby later on. It is also important to avoid infant formula as the first feed, because the baby gets used to that instead of breastmilk. And nurses need to know techniques for helping mothers who experience problems with breastfeeding. All of these are addressed in our curriculum.

What are some of the successes you’ve seen?
One of the hospitals we worked with created a special ward once they understood the importance of keeping mother and baby together. And nurses have really become great advocates for breastfeeding. We have prepared “master trainers” among hospital staff to ensure that the trainings will continue. These workers now handle rollout on their own using the manuals and materials we provided.
How have your own experiences as a mother informed your work?
When I had my son in 2018, I planned to breastfeed him exclusively. But my delivery was a Caesarean, and the hospital had a policy of separating newborn and mother for fear of infection. I was confined to the post-op ward for 18 hours without my family! When my husband was finally allowed in, I asked him to have the nurses bring our child so I could breastfeed. They refused, and only much later was my son brought to me.
I felt very guilty and thought, “How can I go back to work and say that my baby’s first feed was formula?” I really needed support, but the nurses only said, “The baby’s not suckling. He is lazy.” It was very frustrating. When we got home, my sister-in-law, who was still breastfeeding her two-year-old son, helped my baby learn how. Gradually I was able to increase breastfeeding on my own, and by the time I returned to work, my son was completely off formula.
Now when I train health workers, I always tell my own story.
This experience made me an even stronger advocate. Now when I train health workers, I always tell my own story.
What other nutritional challenges do infants and young children face in Nepal?
Nepal has already shifted from traditional, staple foods to a diet that is high in sugar, salt, and fat. In studies we conducted in 2017, we found that children are consuming more unhealthy packaged foods from markets, in part because of changing lifestyles and more urbanization. People see this processed food as “fancy” — eating it increases social status.
Formula also has become an “easy way out” for mothers and health workers. Fortunately, we aren’t seeing as much marketing of formula in Nepal as in other countries, but formula is seen here as a part of that “fancy” lifestyle.

You can help ensure more families have the resources they need to create lasting change in their own lives.